Gastroschisis is the intrauterine evisceration of
fetal intestine through a paraumbilical anterior abdominal
wall defect, nearly always on the right side of the
umbilicus. In addition to the evisceration of the
intestine
the stomach, bladder and gonads are often extra-abdominal.
The liver does not herniate from the defect. There
is
no surrounding sac and so the intestines are exposed
to the amniotic fluid during pregnancy. The bowel
usually
becomes shortened, thickened and dilated and is often
matted together with adhesions.
Gastroschisis is thought to originate from a relatively
late event in development since there are few associated
anomalies. It may arise from an isolated vascular event
involving the right side of the abdominal wall. This
abnormality occurs sporadically and has a low recurrence
rate. It is therefore extremely doubtful that a genetic
cause is responsible for gastroschisis so the possibility
of a nutritional or environmental aetiology remains.
Associations with young mothers and low social class
are established but not understood. Smoking has been
suggested as a possible risk factor and an increased
risk for gastroschisis has been described in women
using
recreational drugs before or in early pregnancy.
Go to the top of this
page
ANTENATAL
In gastroschisis the maternal serum AFP level is
elevated in approximately 75% of cases, values of 4-5
multiples of the median are common. The diagnosis is
made on ultrasound by visualising the free loops of
bowel that herniate through the anterior abdominal
wall into the amniotic fluid. Click
for picture 
Although the risk of aneuploidy is low, a detailed
ultrasound examination should be performed with early
karyotyping if indicated. Cases of ruptured exomphalos
have been reported and can be confused with gastroschisis.
Serial ultrasonography allows the measurement of
fetal growth and intestinal assessment looking for
dilatation and abnormal peristalsis. The amniotic fluid
is either normal or slightly diminished unless there
is associated gastrointestinal atresia when polyhydramnios
may develop. Consideration should be given to fetal
assessment with umbilical artery Doppler velocimetry
because of the association with stillbirth.
Go to the top of this
page
POSTNATAL
The choice of timing, mode and unit of delivery are
controversial. There is a balance between the ultrasound
findings of the bowel and indices of fetal well-being
with the risks associated with preterm delivery. A
vaginal delivery should be contemplated unless there
is an obstetric contraindication. Immediate postnatal
treatment includes resuscitation, transfer and operative
reduction.
In gastroschisis, survival is around 90% and at least
80% have a single operation to repair the abdomen.
The umbilicus is usually preserved. Forcing the intestines
into too small an abdominal cavity can affect ventilation,
vascular blood supply and renal perfusion. If this
is the case a silo is fashioned and delayed closure
performed after gradual reduction over 3-10 days. This
is necessary if the abdomen is small particularly in
the baby with intrauterine growth retardation. Patients
require intravenous nutrition with normal feeding established
in most cases at between 20 and 40 days but support
may last for 6 or more months.
Go to the top of this
page
WEST MIDLANDS
DATA
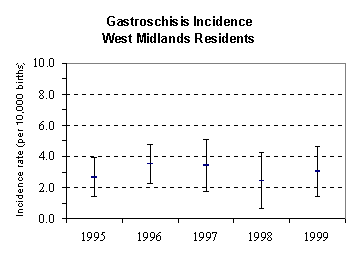
Go to the top of this
page
|